
Temple Hills Office
4302 St. Barnabas Road
Temple Hills, MD 20748
Clinton Office
9131 Piscataway Road
Suite #730
Clinton, MD 20735

More Podiatry Foot Care Articles
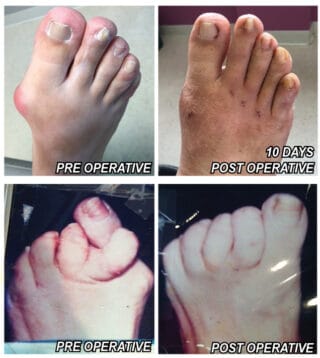
Minimally Invasive Foot Surgery – Permanent Cure For Bunions, Hammertoes and Calluses
You only get one pair to last a lifetime, and most people will clock over 70,000 miles on a pair of feet in a 70 year life span. Mechanically, the feet are one of the most complex parts of the body. There are 26 bones, 30 joints, 19 muscles, and 107 ligaments in each foot. These structures work together to allow the foot to move in six different directions to produce each complete step.
It has been estimated that 80-85% of the general population will suffer from a foot problem at some time in their life. In the past, many foot pain sufferers have avoided permanent cures, opting for periodic palliative care. In the long run, for the active person in pain, this may not be the treatment of choice. These visits may be time consuming, expensive, and will not permanently cure a problem that may worsen.
How Minimally Invasive Surgery Differs From Traditional Foot Surgery
Minimally Invasive Surgery (MIS) is a technique which enables a specially trained and certified surgeon to eliminate most bunions, hammertoes, corns, calluses, and spurs through a small incision often requiring only one stitch, so no big scars. The procedures are performed with small specialized instruments with a diameter about the same size as a pen point. The boney structures are viewed during surgery by use of a Flouroscope, so even though the incision is small, the surgeon can visualize the structures he/she is working on at all times during the surgery.
Unlike other surgeries, major factors associated with MIS are different. There is no hospitalization or deep general anesthesia required. The surgery is performed in a certified Ambulatory Surgical Center under local anesthesia with IV sedation administered by an anesthesiologist or a certified nurse anesthetist, so the patient will experience no pain before or during the surgery. Following the surgery, the patient will leave walking, be instructed to go directly home and remain off the foot other than ambulating to the bathroom for 2448 hours. The recovery time, and post-operative pain, swelling, and risk of infection is usually diminished with MIS due to the small incision, less exposure time, and lessor amount of soft tissue dissection and trauma to the structures. With some procedures, patients are often able to return to sedentary jobs in 23 days.
Etiology
The most common cause of bunion deformities is believed to be a combination of hereditary tendencies and biomechanical imbalances. For example, excessive pronation, commonly referred to as flat-feet, places excessive stress on the inside of the big toe during toe-off forcing it into a valgus direction toward the smaller toes. As the bunion develops, the head of the metatarsal bone enlarges, becomes more prominent, and is irritated by the shoe. This can be demonstrated with the hand by holding the palm flat against a table and slowly bending the hand and watching the knuckles become more prominent.
Treatment
The first choice in the treatment of bunion deformities is to discover them early in life so a conservative, mechanical approach may be used. This may include orthotics or a minimally invasive flatfoot correction. However, once the great toe is deviated and the metatarsal bone becomes prominent enough to be symptomatic in shoes, the only permanent cure is surgical correction, which in the majority of the cases can be done through the minimally invasive technique.

















